Sleep Apnea Recovery Stories- Life after tracheostomy: One man's successful fight with sleep apnea
We like sharing stories from people like you and me. People who are either struggling with sleep disorders or those who have overcome them.
In today’s story, we share Mike’s successful story of how he overcame sleep apnea by getting a tracheostomy surgery.
Mike will take it from here
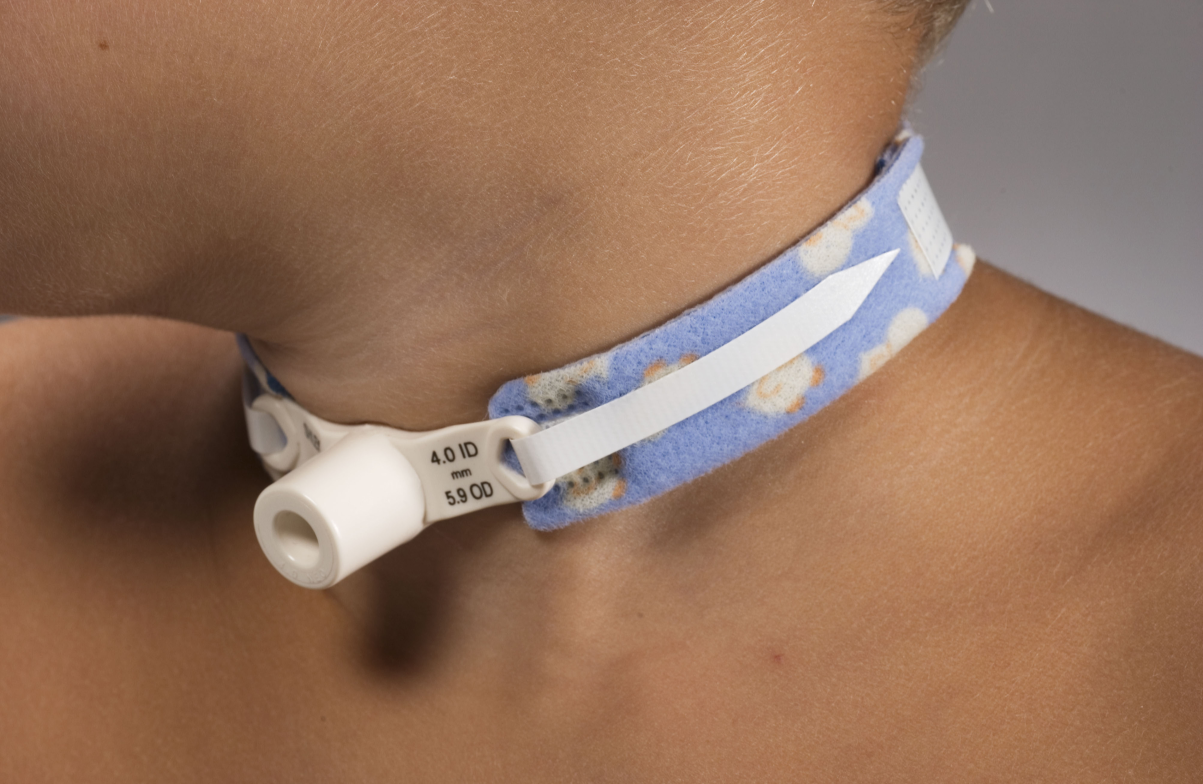
“My name is Mike and I recently underwent tracheostomy surgery to treat severe obstructive sleep apnea.
I was diagnosed with sleep apnea several years ago and was immediately set up on a CPAP machine. After losing one job and reaching the breaking point on my current job, I sought help and realized that I had neglected treating my sleep apnea and it was destroying my life.
My sleep apnea got so bad that I was experiencing some very perturbing symptoms. My snoring was keeping my wife, Beth, awake and she would leave the bedroom at times to work in the middle of the night and sometimes fall asleep on the couch.
I was waking up at least once every hour to go to the bathroom. When things got really severe, I had an occasional bladder accident which I have now learned is not uncommon in severe sleep apnea cases.
I was a zombie day and night. I slept at my desk 3 hours a day on a good day and 5 hours a day on a bad day, and the bad days were more numerous than good.
I went to another doctor, had another sleep study, received a new pressure setting for my CPAP machine and started taking my treatment seriously.
The setting was an extreme 22 cm, and I was not able to tolerate it. I woke up with earaches and a sore throat. One of the more embarrassing problems of the high pressure was waking up with a bloated stomach and then loudly belching non-stop for 20 to 30 seconds.
After several months of aggressive treatment, the doctor determined that CPAP had failed. It was at that time I requested a tracheostomy.
I had studied the surgical alternatives for my condition and came to the conclusion that due to the severity of my obstruction, and with my goal of being free of CPAP, the only surgery that might help me would be the trach.
I had my surgery July 14th, 2012. Since that time I have been counting my blessings. I have experienced only low to moderate pain. I have healed quickly and the drainage from the surgical site stopped by the 9th or 10th day.
Life after the surgery
The results of the surgery … I SLEEP LIKE A BABY!
I took a couple of days to adjust to getting a full night’s sleep. The first two nights I would wake up after 2 hours wide awake and ready to start the day. I have adjusted, though, and now sleep 7 to 8 hours a night without any problem. NO SNORING, NO APNEA; just peaceful sleep. I have had small things that woke me up, like the drainage or pain, but that is getting better and I am so thankful.
During the day I am awake! I am alert and can concentrate again. I have also noticed that I am doing more work around the house. I am also happy to say I passed one major test. Last Sabbath I went to church and STAYED AWAKE THROUGH THE WHOLE SERMON! I am really counting my blessings.
6 months down the line
It tracked my progress for 6 months since my Tracheostomy surgery.
I had pretty much healed after my surgery and things were going well. Then one night I had a coughing fit. After the fit was over I was brushing my teeth and suddenly I couldn’t breathe. I gagged and fought to breathe but I was somehow obstructed. I opened my trach tube and stumbled to the bedroom. “Help me!” I whispered to my wife and we quickly got dressed and went to the emergency room.
I was quickly ushered into the examination room and the doctor soon arrived. He was obviously not well versed in tracheostomies and had no idea what to do.
He had me hooked up to a nebulizer to see if he could soften anything that was stuck. That didn’t work so he order a muscle relaxant to see if my muscles in my throat were doing it. That didn’t work either.
My wife drove home to get my trach information to show the doctor. As the doctor saw other patients, I read the papers and in the troubleshooting section read that if you have breathing trouble make sure the tube is turned to the correct position.
I twisted the tube and VIOLA! I could breathe. Now I know that the notch on the bottom of the tube must be facing down, not up.
The next story is less exciting but was still a major annoyance. I was showering and some shampoo ran down over my trach tube. That is usually no problem but this time my plug fell out and I breathed soap and water in.
EEYWEE that hurt and I was coughing and spittin’ and I put the plug back in. I coughed and the plug shot out, wet and slippery it wouldn’t stay in and I breathed in more water and shampoo. I grabbed a towel and after throwing up and coughing a lot I dried off the plug and put it back in. I am very careful to make sure my plug is in before I shower and that way showers are no problem…learned the hard way.
The last story is related to being careful not to touch the trach tube with unwashed hands. Use a q-tip whenever possible to clean away anything around the tube. I learned this after a major strep infection.
My wife was not feeling well. I think I got the bug from her and my throat started to swell. The site turned red and my temp soared to 104 degrees. I was out of work for a week and it was miserable.
NOW THE GOOD STUFF!!!
Yes, I had some difficult experiences but I would never give up my tracheostomy. Since my surgery, I have lost 65 lbs. I have not dieted at all and have had enough energy to start lifting weights again. I sleep like a baby and am alert and awake at work and throughout the day.
I am doing things around the house and my marriage is much happier now that I have energy… :-)
I have also had the opportunity to teach other people about the effects of sleep apnea and to give information to help people who have become discouraged because of the destructive effects of OSA on their lives.
I have had some curious stares but that is generally when I am not looking. No one has been rude or stared at me to the point that I would become uncomfortable.
After months of studying and weighing the options I am glad I chose the tracheostomy…it was the right choice for me.
Four Years Later
I will soon celebrate my 4-year anniversary since my tracheostomy surgery and I wanted to share how everything has been going.
I have had a mixed experience with my trach. I am sooooo happy I got the trach and would never go back to living without it.
Memory:
I have to report that my memory has gotten better now that I am getting sleep and oxygen at night.
I am sad to say, though, that my memory is not fully recovered and is not at a level that I would expect for a person my age. I still have trouble remembering some things, and if I am sleepy, it gets worse.
But I am still better than I was before my surgery and I hate to think how bad I would be if I had not gotten my trach.
Infections:
I have had probably a dozen infections in the past 3+ years. Most were mild infections that required an antibiotic. However, I have had two infections that were so nasty that I was genuinely scared about what might happen to me.
The first was a strep infection that hit me like a ton of bricks. I was feeling tired but not really sick. My wife and I were walking down the aisle of an antique warehouse when it hit me and I felt like I was going to fall over.
In a day I was so sick I was just plain miserable. I had a 105 degree fever one day and then went to the doctor for a prescription. The doc did a culture and discovered it was strep.
The second infection that was really nasty was a slow-growth, antibiotic-resistant mycoplasma something or other. Turns out this infection is rare and virulent.
I had a PICC line inserted in my arm. This is a catheter that is threaded through your arm, past your shoulder and into your heart to deliver medication 24/7. I had a pump I carried around for roughly 6 weeks and my doctor was threatening to pull my trach.
I was terrified at the thought of pulling my trach. I could not imagine life as a zombie again and I would get depressed at just the mention of going back to that life. I told my doctor that I was ready to do anything to keep my trach … my sleep apnea would destroy my life and I would surely lose my job.
Eventually, the infection cleared up and luckily I had insurance to pay for it. That infection lasted 10 months and cost a total of roughly $20,000 to treat. I thank God that I had insurance at the time.
I have learned the hard way to never touch my stoma with my finger. I always use a tissue or cotton swab to touch my stoma. I also switched to a new trach tube that is easier for me to clean and I have not had any infections for several months now.
New Tracheostomy Tube
I have switched from my Montgomery Cannula to the Hood Stoma Stent. I find the Hood is more convenient since it is one piece of silicone rather than a tube, an O-ring, a face plate, etc. The Hood is one piece and that helps. The Hood is also flatter on my chest, so now I can wear a tie and close the collar of my shirt.
However, the Hood also can be coughed or pulled out easier, and so I have had to learn how to reinsert the tube myself.
But this is a very good thing. I have accidentally pulled my trach out a few times and each time had to go to the ENT to have it reinserted.
I love my ENT and his office people are great, but I can’t afford to pay for him to reinsert it every time I accidentally pull it out. I have learned how to reinsert it myself now … YIPPPEEEE.
Career
I have to say that my job situation is … good and bad. I have not been able to get a job as a computer programmer, which is what I was trained for. I had some very good job interviews, but as soon as they got a glimpse of my trach, I noticed that their demeanor changed and they never called me back to offer the job to me. I have been forced to change my line of work.
I am now a home caregiver. I have found, though, that in spite of the fact that I do not have insurance or vacation days, I still love this work and do not miss sitting in front of a computer all day.
Frequently Asked Questions
Q: Why did you choose a tracheostomy over other surgeries?
A: I studied the surgeries available for the treatment of Severe Obstructive Sleep Apnea and the trach seemed to have the highest success rate. I also wanted to be free of the CPAP machine, and the only surgery that can accomplish that goal (in my opinion) is the tracheostomy.
Q: How painful was the surgery?
A: I experienced very little pain immediately after the surgery. I compare it to a moderate headache. Also, the pain medication kept the pain in check.
Q: What kind of anesthesia did they use for the surgery?
A: The trach surgery is generally done under a general anesthesia. My doctor had an anesthesiologist do the general. I requested an anesthesiologist rather than a nurse anesthetist because I read that surgery on people with sleep apnea can have additional concerns due to breath stoppages.
Q: How long did it take for you to heal?
A: I was generally healed up by 7 days after the surgery. I was still draining a bit, but it was almost stopped by 7 days.
Q: What do you have to do to care for the trach tube?
A: After the surgery I had to clean around the tube with a Q-Tip dipped in hydrogen peroxide. I was told to suction the tube out often, but it was clear, so I only suctioned it when it became clogged.
Q: Does your voice change in terms of clarity or loudness? I usually have to speak a great deal and at times talk very loud. Is there a change?
A: My voice has not changed. When I put the plug in the tube during the day, my voice is normal. Regarding singing, I sang in church last Sabbath and didn’t have any problems. I have not really tested it with yelling or anything like that. If I take the plug out I can still talk but it sounds really airy and I can only speak 3 to 4 words on a good breath.
Q: What is the difference in sleep quality?
A: This is the reason for the surgery and there is no comparison. I sleep like a rock now. I may wake up once to go to the bathroom or adjust the humidifier I am using at this time, but other than that I am out cold. I have also noticed a big difference in daytime wakefulness and alertness. It is great to have my concentration back.
Q: Do you have a “significant other” that feels more secure with the trach than the CPAP? My wife hates the idea of the machine but cannot stand the idea of being without it and losing me.
A: Yes. My wife and I have been together for the past three years. She has watched my OSA go from bad to worse. She was kept awake by my snoring and fear when I stopped breathing. When I got the CPAP, she woke up when I would tear off the mask, etc. My sleep apnea was extremely severe at one point, waking up every hour, and at one point I was having small bladder accidents.
Since my trach surgery that is all gone and my wife commented that she is getting more sleep now.
Q: Can you wear a suit with a tie during the day?
A: Depends with the type of trach that you have.
For the conventional trachs, ties are a no. You don’t want to push the tube back in. Before I got the Hood Stoma Stent, I would purchase some of those shirts with the really small collar like a priest’s collar. I guess they are called a “collarless dress shirt.” I know some have told me that you can use bolo ties too. It also depends on where the doctor puts the tube. Mine was very low, so it was partially hidden by almost any normal shirts.
Q: Does it affect the outlook for promotion in your line of work? (“We can’t promote him, he has a hole in his throat!”)
A: This one has two answers. I lost my first job after 8 years due to sleep apnea. I was so tired I couldn’t keep up the standard. My current job was on the edge. I was given the choice of go seek help and find out why I was doing so poorly or be terminated. Now that I am awake and alert I see more opportunity for promotion.
Whether there may be some prejudice against us “neck breathers,” I have to say that while it would be illegal, it is still true that people can be intolerant of others who are different than they are. I have not experienced this and hope not to.
I would also have to say that if I miss a promotion, I can live with it better if it is lost due to my boss’ attitude rather than my inability to do the job because of sleep apnea.
Way forward
I have to mention that I am very happy I shared this story. I am so thankful that there were good people out there who helped me when I was considering getting my trach and I am happy I can help those who are now in the place I was.
Also, if you are considering tracheostomy and want to chat, I am more than happy to answer questions and share my experience. Leave your queries in the comment box below. Again, I am not a doctor but it is good to talk with someone who has been there before.
[su_row][su_column size=“1/2”]
Also on Snorezing.com
[su_list icon=“icon: external-link-square” icon_color=“#53eb21”]
- Best rollaway beds
- Best bunk beds with stairs
- Best Snoring Mouthpiece
- Best inflatable Beds
- Best Sleeping Bags
- Best earplugs for sleeping
[/su_list]
[/su_column] [su_column size=“1/2”]
[su_list icon=“icon: external-link-square” icon_color=“#53eb21”]
Sleeping aid Reviews
- Best anti snoring devices
- Best Bedwetting alarm reviews
- My Snoring Solution Review
- Pure Sleep Review
- Best anti snore pillow
- Best Snoring Mouthpiece
[/su_list]
[/su_column] [/su_row]

Patrick Mahinge
With over 10 years of experience in sleep health and consumer reviews, Patrick Mahinge helps you find the best mattresses, pillows, beds, and snoring aids through in-depth testing and expert analysis.
Related Articles


Mouth Breathing Treatment: Stop Mouth Breathing with 7 Easy Everyday Tips
Read more about this article...
Read the Full Feature →
9 common sleep disorders in children & what you can do about them
Read more about this article...
Read the Full Feature →